What is a Root Canal?
Root canal treatment, also known as endodontic therapy, is a procedure that is performed to remove infected or damaged pulp from inside a tooth and replace it with man-made materials. The pulp is the soft tissue inside a tooth that contains nerves and blood vessels. When this tissue becomes infected or damaged, it can cause severe pain and lead to the eventual loss of the tooth if left untreated. Root canal procedures are often the last resort to save a tooth that would otherwise need to be extracted. Ideally, a dentist will be able to catch the infection before it reaches the pulp and treat it with a filling, or a patient will clean their teeth regularly enough to avoid the infection altogether.
When do I need a Root Canal?
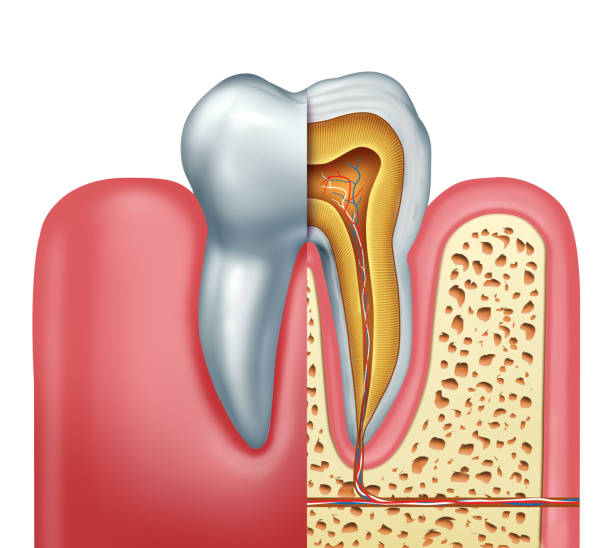
To understand when you might need a root canal, you first have to understand the anatomy of the teeth. A tooth is made up of 2 parts; the crown, which is visible above the gum line and the root, which sits below the gum line.
Additionally, teeth also consist of the following:
- Enamel: The hard outer layer that protects the tooth
- Dentin: A softer, yellow-ish layer underneath the enamel
- Pulp: Soft tissue at the center of the tooth that contains nerves and blood vessels
When a large cavity develops, it can reach past the enamel and dentin and start to affect the pulp. This can cause the nerve endings to become exposed and very painful. Root canals are usually recommended when the infection has spread to the pulp and is causing significant pain.
Early Signs of Needing a Root Canal
Early signs that a root canal may be needed include:
- Pain when eating or drinking hot or cold food and drink
- Pain when biting or chewing
- A loose tooth
Later Signs of Needing a Root Canal
As the infection spreads among the roots, it will eventually kill the nerve, making the pain go away. However, the infection is still present and needs to be treated in order to save the tooth. At this point, common signs of needing a root canal include
- Pain when biting or chewing returning
- Swelling of the gum near the affected tooth
- Pus oozing from the affected tooth
- A swollen cheek or jaw
- The tooth becoming a darker colour
What are the Steps in a Root Canal?
A root canal procedure is typically carried out by a dentist, but in some cases, a patient may be referred to a specialist endodontist. The procedure typically takes place over 2 or more appointments and is usually performed under local anesthesia to numb the affected tooth and surrounding gum tissue (See more about how long a root canal takes). The steps of a root canal are as follows:
Step 1: X-Rays and Examinations
Before the procedure, the dentist will take a series of X-rays to determine the extent of your cavity and the canals of your roots. They may also use visual and tactile methods to assess the area. This will allow them to plan the best course of treatment and decide if treatment is even needed.
Step 2: Numbing the Area
The dentist will then numb the affected area using local anesthesia. Local anesthesia is administered to numb the tooth and surrounding area to ensure the patient does not feel pain during the procedure. The most common local anesthetics used in dentistry include lidocaine and articaine.
Step 3: Isolate the Area Being Worked On
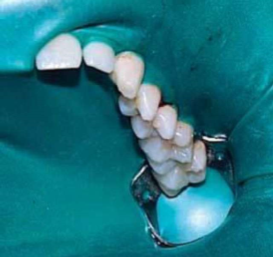
During the procedure, all dentists will place a rubber sheet, called a rubber dam, around the tooth to keep it dry and prevent the patient from swallowing or inhaling any chemicals used during the treatment. This is a safety measure to ensure the patient is not exposed to any hazardous materials and prevent the oral environment from affecting any materials used.
Step 3: Make an Access Hole in the Tooth
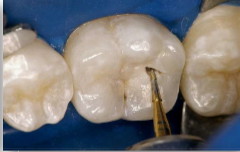
The dentist will then use a drill to go through the harder enamel and dentin surfaces. They will then access the soft tissue inside the tooth, known as pulp, and completely remove it from the crown and roots of the tooth. If there is a dental abscess (a pus-filled swelling) present, the dentist may drain it at the same time.
Step 4: Cleaning and Shaping
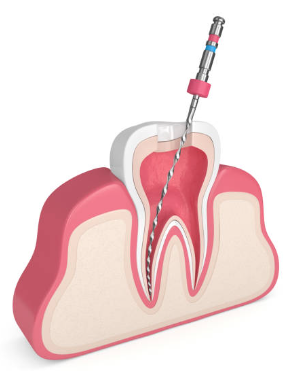
The canals are cleaned and shaped to be filled. The dentist uses a series of progressively larger files to enlarge and shape the canals, ensuring all debris and infected tissue are removed.
Step 5: Disinfection
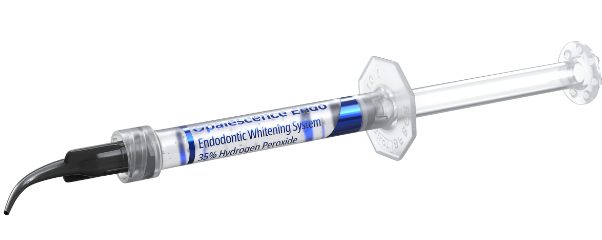
The canals are disinfected with antimicrobial solutions to eliminate any remaining bacteria and prevent further infection. Typically, the disinfectant is hydrogen peroxide, or bleach. While some patients might be considered, this is completely safe if done carefully.
Step 6: Filling the Canals
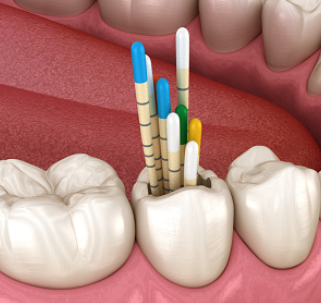
Once cleaned and shaped, the canals are filled with a biocompatible material, usually a rubber-like material called gutta-percha. The gutta-percha is placed with an adhesive cement to ensure a complete seal of the root canals.
Step 4: Temporary Filling
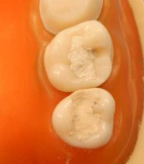
A temporary filling is placed in the access hole created in the crown to seal the tooth until the permanent restoration can be placed. The picture above is an IRM temporary filling, sometimes referred to as a “medicated filling”. It contains eugenol, which has antibacterial properties to help kill any remaining bacteria, however, at the expense of being a weaker material that is more prone to breaking.
Step 5: Permanent Filling/Crown
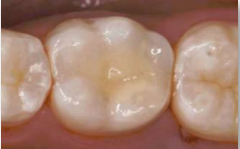
At the next appointment, the dentist will remove the temporary filling, any medication in the tooth will be removed, and the root canal will be filled and sealed. Root-filled teeth are more likely to break than healthy teeth, so the dentist may suggest placing a crown on the tooth to protect it (See more about needing a crown after a root canal).
What to do After a Root Canal?
Root canal recovery is generally straightforward and relatively painless. After a root canal, it is important to take appropriate steps to make sure that the root canal lasts long and prevent any further infections which may lead to the requirement of root canal retreatment.
This includes brushing twice a day and flossing every day, as well as visiting the dentist for regular check-ups. It is also important to avoid any hard foods or anything that may put extra pressure on the tooth between your initial and final treatment days (See more about eating after a root canal).
Driving is usually allowed after a root canal procedure unless otherwise instructed by a dentist. Smoking is generally discouraged after a root canal.
If you experience any pain, feel free to take any over-the-counter pain relievers to help with any discomfort. This includes ibuprofen and acetaminophen. However, if you experience severe pain or swelling after a root canal, contact your dentist as soon as possible.
Conclusion
In conclusion, root canal treatment is a procedure that is performed to remove infected or damaged pulp from inside a tooth. It is a common procedure that is typically performed by a dentist and is often the last resort to save a tooth that would otherwise need to be extracted. The procedure is usually performed under local anesthesia and takes place over 2 or more appointments. Root canal treatment is generally successful, with a high success rate of about 90%. If you are experiencing severe pain or discomfort in a tooth, talk to your dentist about the possibility of a root canal.
Related Articles
Disclaimer
The contents of this website, such as text, graphics, images, and other material are for informational purposes only and are not intended to be substituted for professional medical advice, diagnosis, or treatment. Nothing on this website constitutes the practice of medicine, law or any other regulated profession.
No two mouths are the same, and each oral situation is unique. As such, it isn’t possible to give comprehensive advice or diagnose oral conditions based on articles alone. The best way to ensure you’re getting the best dental care possible is to visit a dentist in person for an examination and consultation.
SAVE TIME AND MONEY AT ANY DENTIST

Less dental work is healthier for you. Learn what you can do to minimize the cost of dental procedures and avoid the dentist altogether!

