Dental implants are a permanent solution for replacing missing teeth. Although it may seem scary aft first, implants can be a great way to restore your smile. In this article, we’ll discuss the different types of implants, implant materials, types of implants, steps in the procedures, risks and complications, cost and more.
What are Dental Implants?
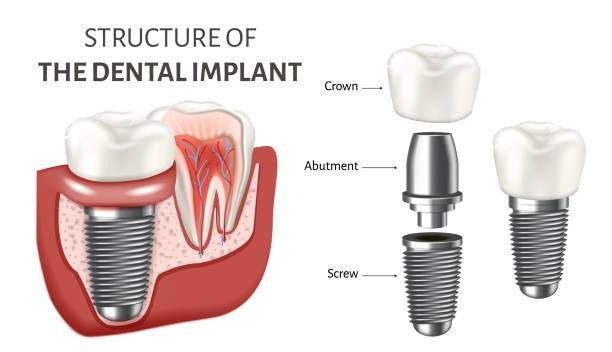
Dental implants are a dental procedure that involves placing a metal prosthesis inside the jaw bone in the space where a tooth used to be. There are various reasons why a tooth may have been removed from the mouth, including decay, injury or gum disease. Dental implants typically consist of a titanium or zirconia fixture surgically implanted into the jawbone. Although dental implants are typically followed by a crown, the implant itself is only the artificial “root” of the new tooth.
Implant Material
The most frequently used dental implant material is titanium. Titanium implants have been around for over 40 years and are the most commonly used due to their ability for osseointegration. Osseointegration is the process by which a dental or orthopedic implant becomes permanently anchored to the bone through various biological and mechanical properties of the implant. This process is critical for the stability and long-term success of the implant. However, if placed incorrectly, it also makes it extremely difficult for a dentist to remove.

Types of Implants
There are three primary types of implants that differ in the way they are placed into your jaw: Endosteal, Zygomatic, and Subperiosteal. Today, typically, only endosteal implants are placed due to the various disadvantages of the other implant types. However, we have included examples of all three implants as some older patients may have previously encountered or used them.
Endosteal Implants
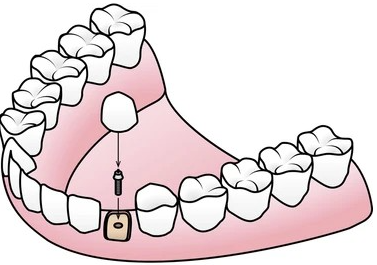
Endosteal implants are the most common type of dental implant. These implants usually have a threaded design, similar to screws, and are the most commonly used type. They are typically made of titanium or zirconia and are suitable for most individuals seeking dental implants.
Zygomatic Implants
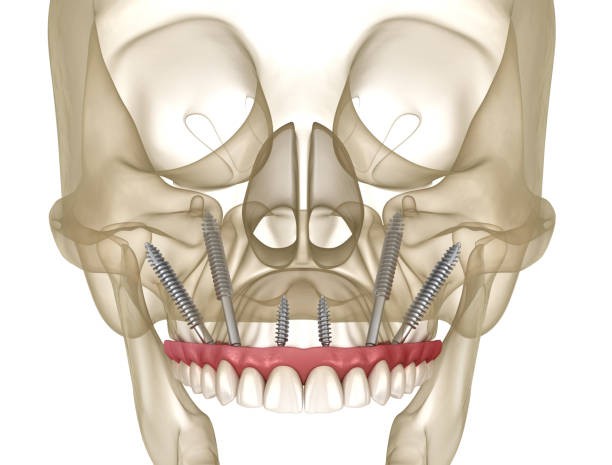
Zygomatic implants are much longer than endosteal implants, placing them in the zygomatic bone rather than the jawbone. The Zygomatic bone (located in the upper jaw) is a larger, sturdier bone than the jawbone, and as such, Zygomatic implants can be used for those who require more support with their implants. That typically means that they are intended for people who have experienced bone loss in the upper jaw. Bone loss can occur due to trauma, medical conditions, or long-term lack of teeth.
Subperiosteal Implants
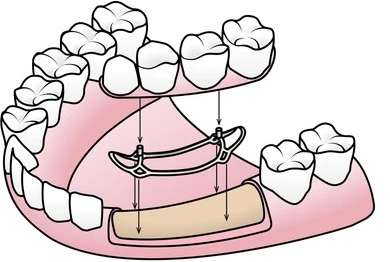
Subperiosteal implants are custom-made metal frameworks that sit on top of the jawbone but underneath the periosteum (the connective tissue covering the bone). Its advantage is that it avoids the need for extensive bone grafting procedures. However, these types of implants have largely fallen out of use compared to the other varieties of implants available today due to their various complications.
Procedure Steps
The procedure for dental implants involves several steps, which we will divide into before, during, and after treatment:
Before Treatment
Before proceeding with a dental implant surgery, your dentist will need to conduct several key steps to ensure the success of the procedure.
- Review Medical History: First and foremost, a dentist must review your medical history is essential to ensure you are able to have an implant. There are various factors, such as metal allergies or bleeding disorders, that may require additional preparation or deem you unsuitable for the procedure altogether.
- Determine if Bone Grafts are Required: Bone grafts are used to increase the volume of available bone in order to secure a dental implant. A bone graft may be necessary if your jawbone has deteriorated due to age or loss of teeth. If the implant is attempted without sufficient bone in your jaw, it increases the chance that it will fail and fall out.
- Determining Implant Size: Typically, a dentist will want to choose an implant that maximizes the amount of surface area with your existing bone without running into nerves or blood vessels. This will allow the implant to have the most stability in the mouth. The exact size of the implant will vary depending on jaw shape and size as determined both clinically and through x-rays.
During Treatment (First Visit)
- Anesthesia is Administered: To ensure comfort and reduce any pain or discomfort, local anesthesia (typically lidocaine or articaine) will be administered before the procedure. Some patients may opt to have general anesthesia while undergoing this procedure; however, local anesthesia is usually all that is needed.
- Incision and Raising of Gum Flaps: This will reveal the bone that your dentist will place the implant into.
- Drilling a Hole for the Implant: To make room for the implant to be placed, a dentist will start by making a small pilot hole, and progressively make it larger to ensure that the bone creates a snug fit with the implant.
- Placement of Implant: Placement of an implant requires just the correct amount of torque. A dentist will use a special handpiece and instruments to properly place the implant in the hole they have created.
- Fixation of Healing Abutment: After placing an implant, a healing abutment can be temporarily placed over your implant. This prevents gum tissue from healing over the implant and prevents a crown from being placed on it.
- Closing Surgical Sight: After the implant has been placed, the dentist will cover the sight and stitch it back closed.
Recovery and Aftercare
After the procedure has been completed, you can expect some amount of swelling or bleeding to occur as your body heals. A few steps must be taken for proper recovery and aftercare. These should be done while you wait for the bone to grow around the implant and lock it into the jaw, which should take 3-5 months.
- Continue to brush and floss twice a day to make sure your oral health remains healthy
- Rinse with water after each meal so that food doesn’t get stuck in the stitches or around the implant
- Avoid brushing vigorously near the surgical area during the first few days after your procedure
- Try not to chew near the implant during the first few days after your procedure
- Stick to soft foods for the first few days after an implant until the area heals
- Take any antibiotics and pain medication if prescribed. If you are in pain but have not been prescribed pain medication, feel free to use Tylenol and Advil
After Treatment (Second Visit)
After the implant has had time to fuse with the jawbone any further crowns or bridges can be attached to your implant. This typically occurs 6 months after the initial implant placement. And that’s it! You’re now ready for a new smile.
Alternatives to Dental Implants
Before considering dental implants, your dentist may recommend other solutions, including bridges or dentures. Although dental implants are usually the best alternative for replacing missing teeth, the expensive cost of dental implants is often a prohibiting factor. In some cases, the following treatment options may also be possible:
- Bridges: A bridge is an artificial tooth anchored to the adjacent teeth that bridges the gap left by one or more missing teeth. It is typically cheaper than an implant but requires adjacent teeth to be extremely healthy as they will be shaven down and bear the burden of an extra tooth.
- Partial dentures: A denture is a removable prosthetic device that can replace one or more missing teeth in the same arch. These are relatively cheap option to replace teeth, but are typically uncomfortable long-term.
- Resin-bonded bridges: Also called Maryland bridges are a type of bridge that is bonded to the adjacent teeth using a resin material. These are quite weak but can be used for front teeth which don’t experience many forces from chewing.
- Flipper: A flipper tooth is a temporary prosthesis used for a single tooth replacement. These are not long-term solutions but they can hide a gap in front teeth while one waits for a permanent solution.
- Orthodontics: The use of braces or aligners to shift teeth into the proper location to fill in gaps created by missing teeth can sometimes be achieved. However, this is only in specific circumstances.
Risks and Complications
While dental implant surgeries are generally safe (with an over 90% rate of success), as with any medical procedure, there are potential risks and complications. Here are some risks and complications associated with dental implant procedures:
- Infection: Bacteria can cause bone and tissue loss around the implant, leading to implant failure.
- Nerve damage: During the procedure, if an implant is placed improperly, nerves can be damaged, leading to numbness, tingling, or loss of sensation in the mouth, tongue or lips.
- Sinus problems: Dental implants placed in the upper jaw can protrude into the sinus cavities, leading to infections and sinus problems.
- Implant failure: In some cases, the implant may fail to fuse with the bone or become loose, leading to its removal.
- Peri-implantitis: This condition results from inflammation of the surrounding gum tissue due to bacterial infection, leading to bone loss around the implant.
- Bleeding: Uncontrollable bleeding may occur in some patients, particularly those with bleeding disorders.
Conclusion
Dental implants are an effective, long-term solution for replacing missing teeth. When properly cared for, they can last a lifetime and provide a realistic alternative to bridges, dentures and other options. However, there are some risks and complications associated with dental implants that should be discussed with your dentist before undergoing the procedure. Ultimately, dental implants may be the best solution for replacing missing teeth with natural-looking results. Talk to your dentist to determine if dental implants are the right choice for you.
Disclaimer
The contents of this website, such as text, graphics, images, and other material are for informational purposes only and are not intended to be substituted for professional medical advice, diagnosis, or treatment. Nothing on this website constitutes the practice of medicine, law or any other regulated profession.
No two mouths are the same, and each oral situation is unique. As such, it isn’t possible to give comprehensive advice or diagnose oral conditions based on articles alone. The best way to ensure you’re getting the best dental care possible is to visit a dentist in person for an examination and consultation.
SAVE TIME AND MONEY AT ANY DENTIST

Less dental work is healthier for you. Learn what you can do to minimize the cost of dental procedures and avoid the dentist altogether!

