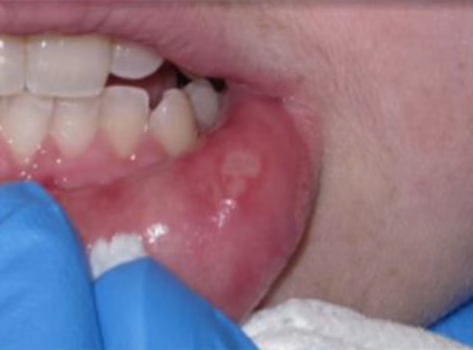
Canker sores are extremely common, affecting about 1 in 5 people, and while they can be painful and frustrating, they are not dangerous. That said, not every mouth ulcer is a canker sore, and knowing the difference matters.
This guide explains everything you need to know inlcuding pictures of what is and isn’t a canker sore and best treatment options.
What Is a Canker Sore?
The medical name for a canker sore is recurrent aphthous stomatitis (RAS).
A canker sore is:
- A painful ulcer inside the mouth
- Not contagious
- Not caused by a virus
- Usually round or oval, with:
- A yellow-white center
- A red, inflamed border
Canker sores almost always occur on movable, soft tissue, such as:
- Inside the cheeks
- Inside the lips
- Under the tongue
- The floor of the mouth
- The soft palate
They do not usually occur on hard, attached gum tissue or the roof of the mouth (with some exceptions).
Why Do Canker Sores Happen?
There is no single cause, but research shows canker sores are related to an immune reaction involving T-cells. In simple terms, your immune system temporarily overreacts and damages the lining of the mouth.
Common triggers include:
Immune-Related Factors
- Family history (strong genetic link)
- Stress
- Conditions affecting the immune system
- Hormonal changes
Weakened Mouth Lining
- Minor trauma (biting your cheek, sharp foods)
- Aggressive toothbrushing
- Nutritional deficiencies (iron, B vitamins, folate, zinc)
- Quitting smoking (temporarily increases risk)
Increased Irritants
- Toothpaste containing sodium lauryl sulfate (SLS)
- Certain medications (NSAIDs, beta-blockers, methotrexate)
- Foods like chocolate, coffee, cheese, gluten, strawberries, preservatives
In many people, multiple factors are involved.
Types of Canker Sores
There are three main types, and knowing which one you have helps guide treatment.
Minor Canker Sores (Most Common)
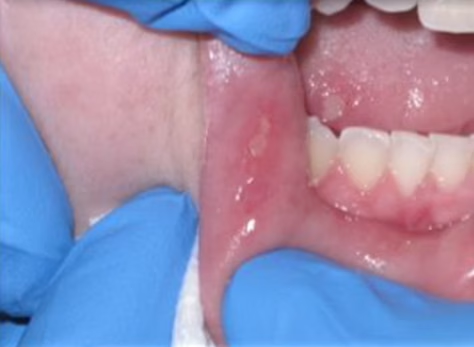
This is what most people mean when they say “canker sore.”
- Small (3–10 mm, under 1 cm)
- 1–5 sores at a time
- Very painful for their size
- Heal in 7–14 days
- Do not scar
- Occur almost exclusively on soft tissue
These tend to come and go over years.
Major Canker Sores
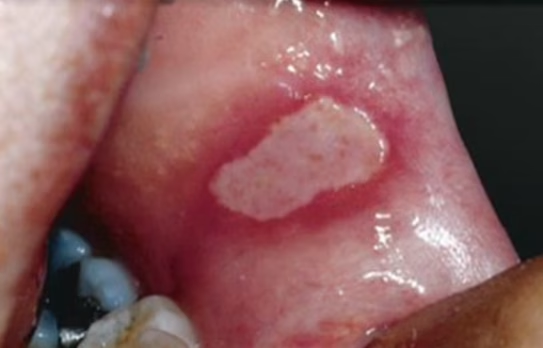
Less common, but more severe.
- Larger (1–3 cm)
- Deeper ulcers
- Often last 2–6 weeks
- Can heal with scarring
- May affect soft palate and throat
- Pain can be significant
These may require prescription treatment and closer monitoring.
Herpetiform Canker Sores
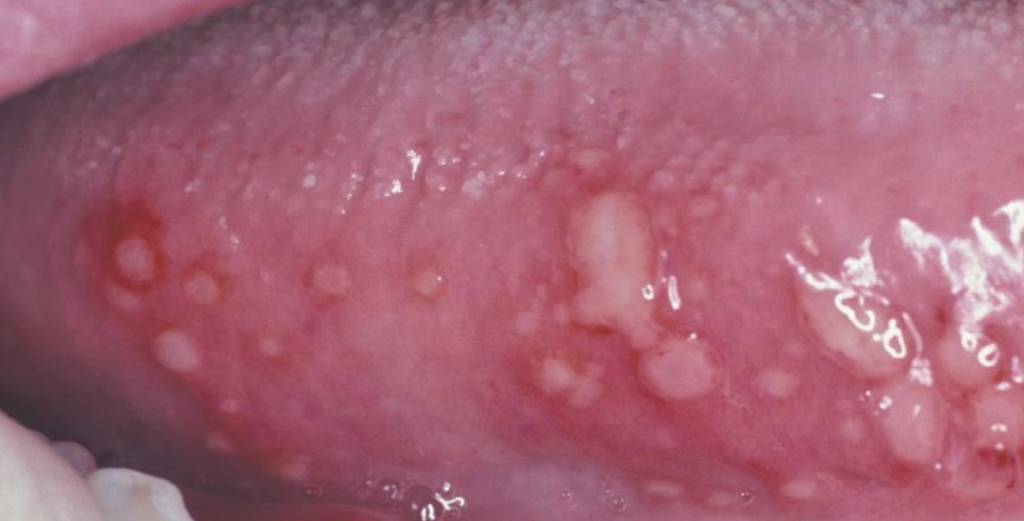
Despite the name, these are not herpes.
- Dozens of tiny ulcers (sometimes up to 100)
- Very frequent recurrences
- Can merge into larger irregular ulcers
- Heal in 7–10 days
- Can occur on almost any oral surface
These often look alarming but are still non-infectious.
What a Canker Sore Is NOT
Many conditions look similar to canker sores. Here’s how to tell them apart.
Cold Sores (Herpes Simplex Virus)
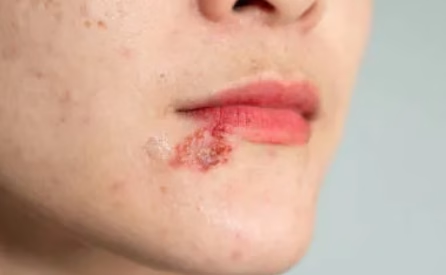
Often confused with canker sores, cold sores are an entirely different entity caused by a viral infection.
- Appearance: Typically start as small, fluid-filled blisters (vesicles) that eventually rupture and crust over.
- Location: Occur on keratinized tissue, such as the border of the lips, the hard palate, or the gums attached to the teeth.
- Distinguishing Clue: They are contagious and often preceded by a “prodromal” tingling or burning sensation at the site.
Erosive Lichen Planus
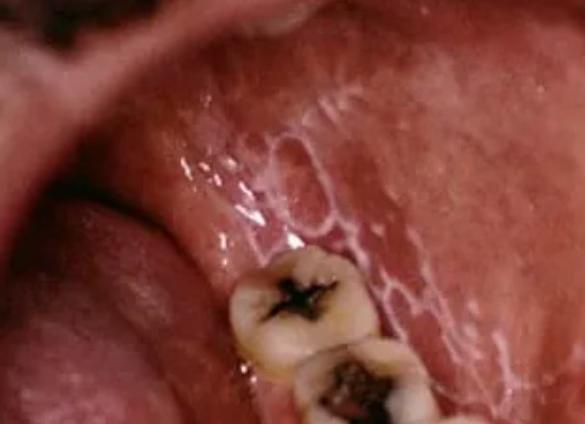
Unlike a standard canker sore, Lichen Planus is a chronic inflammatory disease characterized by relapses and remissions.
- Appearance: Features painful ulcers covered by a whitish pseudomembrane.
- Distinguishing Clue: The ulcers are typically surrounded by Wickham’s striae (fine, white, shiny lines or “striations”) and areas of redness (erythema).
- Location: Most commonly found on the posterior buccal mucosa (inner cheeks) and the tongue.
- Diagnosis: While some forms can be diagnosed clinically, erosive/ulcerative forms require a biopsy for confirmation.
Pemphigus Vulgaris
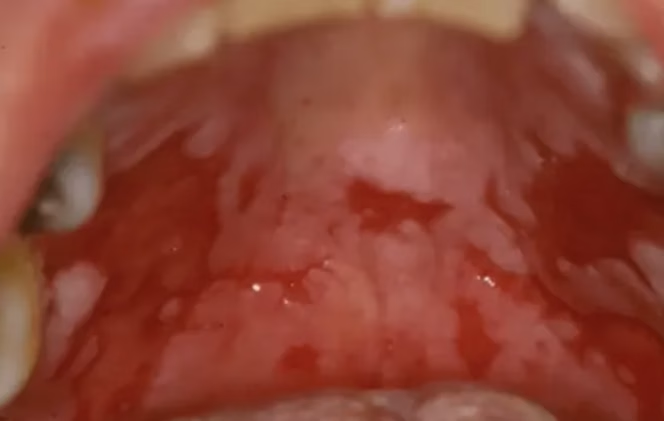
This is a serious, potentially fatal immunobullous disease where the body produces autoantibodies against the “glue” (desmoglein) holding epithelial cells together.
- Appearance: Causes fairly rapid development of thin-walled blisters (vesicles) that rupture into extensive, irregular, and very painful ulcers.
- Distinguishing Clue: Nikolsky’s sign—applying sliding pressure to seemingly normal mucosa causes the epithelium to detach or form a new blister.
- Systemic Risk: Oral lesions are common and are often the first sign of the disease before it spreads to the skin.
- Management: Requires aggressive treatment with systemic steroids and immunosuppressive agents.
Mucous Membrane Pemphigoid
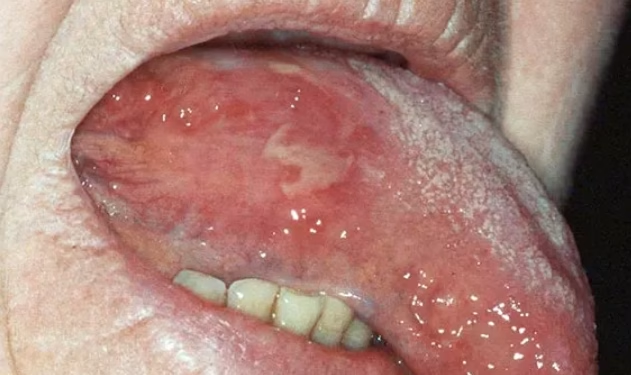
Also known as Cicatricial Pemphigoid, this chronic disease involves autoantibodies attacking the basement membrane.
- Appearance: Characterized by redness (erythema) and thick-walled blisters.
- Distinguishing Clue: It involves the gingiva (gums) in approximately 90% of cases, often presenting as “desquamative gingivitis” where the gums are tender and bright red.
- Major Concern: It can involve the eyes (conjunctiva), leading to scarring and potential blindness.
- Patient Profile: Typically affects older patients in their 6th and 7th decades of life.
Oral Cancer (Squamous Cell Carcinoma)
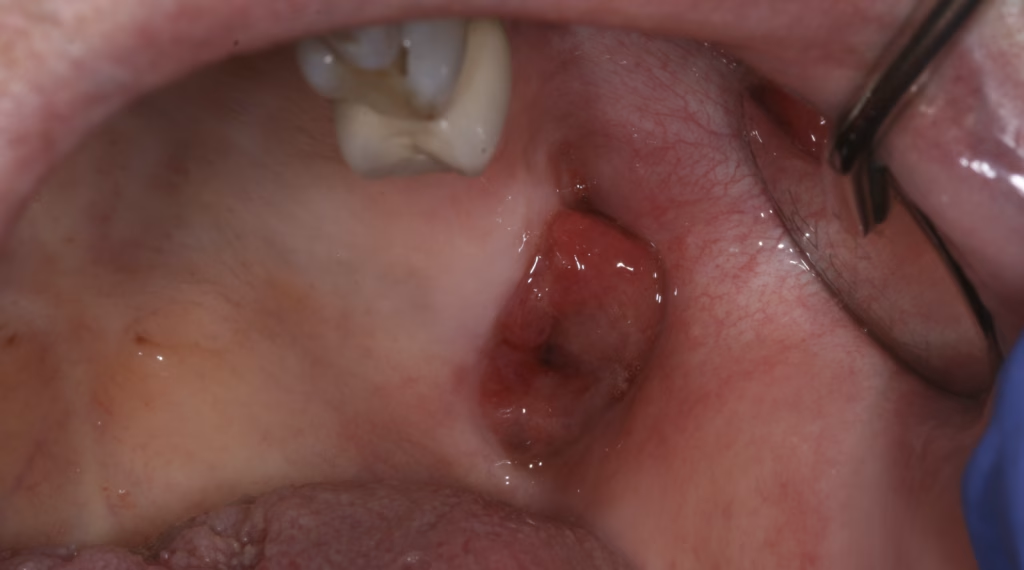
A persistent ulcer can occasionally be a sign of malignancy rather than a simple immune reaction.
- Management: Any suspicious or non-healing ulcer must be evaluated by a professional; a biopsy is the only way to definitively rule out cancer.
- Appearance: Often appears as an ulcer with firm, raised, or “rolled” borders.
- Distinguishing Clue: These ulcers are persistent (lasting more than 2 weeks) and may be associated with unexplained bleeding, numbness, or lumps in the neck.
Systemic Diseases Associated With Mouth Ulcers
Frequent or severe canker sores may be linked to underlying conditions such as:
- Behçet disease
- Celiac disease
- Inflammatory bowel disease
- Iron-deficiency anemia
- Vitamin deficiencies
- HIV/AIDS
- Cyclic neutropenia
In these cases, treating the underlying condition often resolves the ulcers.
What Should You Do If You Have a Canker Sore?
If It’s Mild and Infrequent
- No treatment is required
- Avoid spicy or acidic foods
- Use a soft toothbrush
- Maintain good oral hygiene
- Avoid SLS-containing toothpaste
If It’s Painful or Frequent
- Topical corticosteroid pastes or rinses
- Protective oral gels
- Prescription mouth rinses
- Tetracycline or doxycycline rinses in selected cases
- Laser therapy (in some dental offices)
Silver nitrate is no longer recommended due to risk of tissue damage.
When to See a Dentist or Doctor
- Ulcers lasting longer than 2 weeks
- Very large or deep ulcers
- Frequent recurrences
- Ulcers plus fever, genital ulcers, eye symptoms, or joint pain
- Ulcers that look unusual or don’t heal
Bottom Line
A canker sore is a common, non-contagious, painful mouth ulcer caused by an immune reaction. Most heal on their own, but recurrent or severe ulcers deserve proper evaluation to rule out other conditions.
If you’re ever unsure whether a sore is “just a canker sore,” getting it checked is always the right move.
Early evaluation brings peace of mind — and better treatment.
Disclaimer
The contents of this website, such as text, graphics, images, and other material are for informational purposes only and are not intended to be substituted for professional medical advice, diagnosis, or treatment. Nothing on this website constitutes the practice of medicine, law or any other regulated profession.
No two mouths are the same, and each oral situation is unique. As such, it isn’t possible to give comprehensive advice or diagnose oral conditions based on articles alone. The best way to ensure you’re getting the best dental care possible is to visit a dentist in person for an examination and consultation.
SAVE TIME AND MONEY AT ANY DENTIST

Less dental work is healthier for you. Learn what you can do to minimize the cost of dental procedures and avoid the dentist altogether!

